Introduction
Pemphigus comprises a rare but potentially life-threatening group of autoimmune bullous dermatoses that primarily affect the skin and mucous membranes. Histopathologically, it is characterized by the presence of intraepidermal acantholysis and deposition of IgG autoantibodies against desmosomal cadherins, notably desmoglein 1 (Dsg1) and desmoglein 3 (Dsg3), leading to compromised intercellular adhesion among keratinocytes [1].
Among its subtypes, pemphigus vulgaris (PV) is the most frequent and clinically severe, marked by suprabasal acantholysis and predominant involvement of mucosal surfaces, including the oral cavity [2]. The disease exhibits a global distribution, affecting both sexes equally, with peak incidence between the fourth and sixth decades of life.
Epidemiological data suggest an incidence ranging from 0.75 to 5 cases per million population per year, with notable regional variations linked to genetic and environmental factors [3].
The immunopathogenesis of PV is driven by IgG autoantibodies targeting Dsg3 in mucosal-dominant PV, and both Dsg1 and Dsg3 in mucocutaneous forms [4]. Interestingly, the phenomenon of immunological epitope spreading can result in clinical transformation between pemphigus subtypes, with serological transition from anti-Dsg1 to anti-Dsg3 or from anti-Dsg3 to anti-Dsg1 [5]. Ocular involvement in PV is relatively uncommon, yet when present, it tends to be associated with higher systemic disease activity. The most frequently affected ocular structures are the conjunctiva and eyelid margin [4]. Involvement of the lacrimal apparatus, particularly the lacrimal punctum, remains extremely rare and poorly characterized in the literature [6].
Early recognition of atypical presentations, such as those involving the ocular adnexa, is critical to prevent delayed diagnosis and management, which may otherwise contribute to structural damage or functional impairment [7]. The pathophysiological mechanisms underlying ocular involvement are hypothesized to mirror mucosal PV, where desmoglein-targeted autoantibodies disrupt epithelial adhesion in ocular tissues [8]. Recent literature emphasizes the role of direct immunofluorescence (DIF) and enzyme-linked immunosorbent assays (ELISA) in confirming the diagnosis, while advances in systemic immunosuppressive therapy—particularly with rituximab—have dramatically improved outcomes [9]. Surgical approaches to complications involving ocular structures, although seldom required, must be carefully tailored and reported to enhance the clinical body of evidence [10].
This report aims to contribute to the understanding of PV with rare ocular involvement by presenting a unique case of lacrimal punctum compromise, emphasizing the diagnostic, therapeutic, and surgical considerations.
Case Report
A 51-year-old female patient from Mogi das Cruzes presented with a pruritic lesion, with slow and progressive growth in the upper lacrimal punctum of the right eye for approximately 1 year.
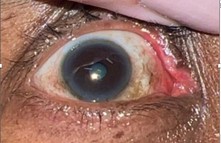
Figure 1. Lesion in the topography of the upper lacrimal canal of the right eye.
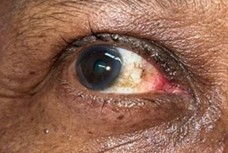
Figure 2. Post-operative appearance.
Surgical excision with reconstruction of the lacrimal punctum was performed, and the anatomopathological examination revealed vesiculobullous dermatosis with chronic perivascular lymphoplasmacytic inflammation in the superficial dermis, with immunohistochemistry suggestive of PV.
Conclusion
Pemphigus is a disease that should be among the differential diagnoses of eyelid lesions, despite its rare presentation. Early diagnosis and treatment are essential for better diagnostic elucidation.
References
2. Femiano F. Pemphigus vulgaris: recent advances in our understanding of its pathogenesis. Minerva Stomatol. 2007 Apr;56(4):215–23.
3. Ishii K, Amagai M, Ohata Y, Shimizu H, Hashimoto T, Ohya K, et al. Development of pemphigus vulgaris in a patient with pemphigus foliaceus: antidesmoglein antibody profile shift confirmed by enzyme-linked immunosorbent assay. J Am Acad Dermatol. 2000 May;42(5 Pt 2):859–61.
4. España A, Iranzo P, Herrero-González J, Mascaro JM Jr, Suárez R. Ocular involvement in pemphigus vulgaris - a retrospective study of a large Spanish cohort. J Dtsch Dermatol Ges. 2017 Apr;15(4):396–403.
5. Hertl M, Jedlickova H, Karpati S, Marinovic B, Uzun S, Yayli S, et al. Pemphigus. S2 Guideline for diagnosis and treatment-guided by the European Dermatology Forum (EDF) in cooperation with the European Academy of Dermatology and Venereology (EADV). J Eur Acad Dermatol Venereol. 2015 Mar;29(3):405–14.
6. Wang HH, et al. Ocular involvement in autoimmune blistering diseases: a systematic review. The Ocular Surface. 2020;18(2):180-9.
7. Kridin K, Bergman R. Ophthalmic involvement in pemphigus: a systematic review. American Journal of Clinical Dermatology. 2018;19(6):797–803.
8. Bascones-Martínez A, Arias-De Santiago S, González-Moles MA. Topical and systemic therapy of pemphigus vulgaris: a systematic review. Medicina Oral, Patología Oral y Cirugía Bucal. 2021;26(3):e345–52.
9. Mimouni D, Nousari CH, Cummins DL, Kouba DJ, David M, Anhalt GJ. Differences and similarities among expert opinions on the diagnosis and treatment of pemphigus vulgaris. Journal of the American Academy of Dermatology. 2003 Dec 1;49(6):1059–62.
10. Ghalamkarpour F, et al. Surgical management of lacrimal duct obstruction in autoimmune disorders: experience and outcomes. Canadian Journal of Ophthalmology. 2021;56(1):20–25.